Welcome, dear readers! 😊
Let’s get straight to the heart of this dental matter. Like it or not, oral health is pivotal to our overall well-being. Yet, many of us tend to overlook the potential threats, such as gum disease.
Did you know that gum disease has more serious implications beyond the health of your mouth? It’s a sneaky cul-de-sac which might even jeopardize the success of our beloved helpmate – dental implants.
In this article, we’re going to look closely at this essential yet often misunderstood condition. We’ll answer questions like: What is gum disease? How does it occur? What is its connection to dental implants?
Plus, we’ll delve into the significant risk factors and provide some insights on dealing with this condition when considering dental implants. So, brace yourself! We’re about to embark on an enlightening journey into the world of gum disease and its link to dental implants. Stick around! 🌟
Table of Contents
Overview of Gum Disease
Gum disease, known formally as periodontal disease, is one of the most under-recognized yet far-reaching health issues we face today. As a silent crisis, it doesn’t receive the attention it deserves, not considering its shockingly high prevalence and severe effects on oral health.
Prevalence in the Population
Think about the people you know – family, friends, colleagues. Now, can you believe that approximately 47.2% of Americans over the age of 30 have some form of gum disease? That’s almost half of the adult population! 😲 And the situation only worsens with age, with a staggering 70.1% of adults aged 65 and older battling gum disease. That’s more than 2 in every 3 seniors!
But instead of scaring you, we want you to realize how prevalent this issue is. Since many of us have the misconception that oral health issues are rare, these statistics serve as a wake-up call.
Effects on Oral Health
Beyond these facts and numbers, let’s take a closer look at how gum disease affects our oral health and overall well-being. Primarily, tooth decay and gum disease affect 38.4% and 32.3% of adults respectively, making them two of the most common oral health issues.
Gum disease might start as a mild inflammation of the gums (gingivitis), but if left unchecked, it can advance to a severe form known as periodontitis. This ailment can damage the soft tissue and bone that support your teeth, eventually leading to tooth loss. 😔 Severe cases are a leading cause of tooth loss in adults.
Moreover, gum disease doesn’t always stop at your mouth. Inflammation can potentially extend to other parts of your body, contributing to heart problems, diabetes, and mood disorders such as depression.
These stats and potential effects underscore the need for maintaining proper oral hygiene, regular dental check-ups, and getting professional periodontal care when necessary. Speaking of periodontal care, Periodontal Dentistry in Los Angeles is renowned for its world-class care and specialized gum disease treatments. It’s time that we put our oral health in the spotlight and make gum disease a conversation everyone is a part of. After all, our mouth is the gateway to overall health, and we deserve to keep it sparkling! 😄
Dental Implants and Their Success Rate
Allow us to cast your doubts on dental implants aside and serve you with peace of mind. Dental implants don’t merely rejuvenate your million-dollar smile after tooth loss; they’re a health investment with a whopping 95% success rate, making them a tried-and-true solution. If you’re toying with the idea of dental implants, continue reading to better understand why they’re a smart choice.
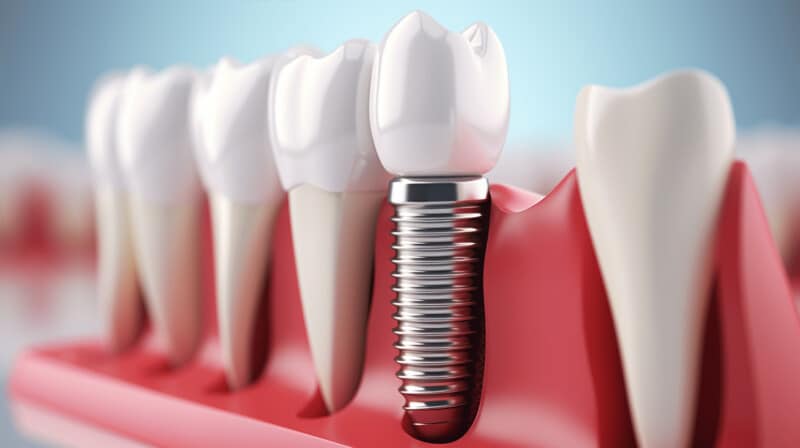
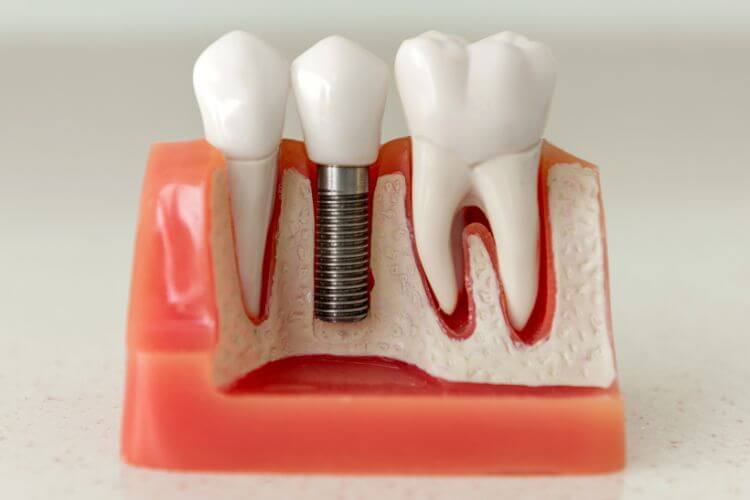
First off, let’s debunk any misunderstandings about dental implants. 😊 They are artificial tooth roots, almost similar to your natural ones, installed with precision into the jawbone. Once in place, a tooth-like dental crown is fixed atop, offering the same strength and aesthetic appeal as your natural teeth.
Interestingly, the astounding 95% success rate of dental implants isn’t accidental; it’s due to several reasons:
- Biocompatibility: Dental implants are made of titanium, a material well-tolerated by our bodies. This reduces chances of rejection or allergic reactions, and fosters osseointegration (fusion of bone and implant).
- Technological advancements: Modern 3D imaging and digital modeling provide accurate and personalized implant placement.
- Prevent Bone Loss: Unlike traditional methods, implants stimulate the jawbone similar to natural teeth, preventing bone loss in the long run.
Of course, every dental procedure has its considerations, and implants are no exception. A point to note is that not all patients might be suitable for dental implants, as factors such as general health, jawbone density, and lifestyle can affect its success rate. Hence, a thorough dental health check-up and consultation with an experienced dentist is crucial before opting for dental implants.
The comfort of dental implants lies in their design, purpose, and high success rate, making them more than just an aesthetic substitution but also a functional asset to oral health. 🦷
In essence, the benefits of dental implants reach far beyond their physical appeal, and their 95% success rate only adds fuel to their popularity. They’re a permanent solution equating to a long-term pledge to your oral health, resulting in a perfect, worry-free smile for years to come. 💖
Peri-Implantitis and Dental Implants
Taking care of our teeth is something we’re all familiar with – a task that becomes even more vital when we have dental implants. Yet, due to a variety of factors, an infection known as peri-implantitis can develop around these implants. This infection could lead to gum inflammation, bone loss, and ultimate implant failure. Understanding this infection, its prevalence, causes, and risk factors can aid us in maintaining our precious smiles 😃.
Prevalence and Causes
Peri-Implantitis, unfortunately, is not an uncommon issue. Statistics show that as many as 56% of patients with dental implants might develop this infection. In addition, nearly 12% of dental implants are affected by gum diseases that could edge on peri-implantitis. That’s a substantial number of beautiful smiles at risk! 😱 So, what causes this ailment?
Dental plaque, the sticky film of bacteria that form on our teeth when we don’t brush and clean them adequately, is a significant cause of peri-implantitis. When this plaque hardens over time, it forms tartar that houses even more bacteria. This unwelcome bacterial ‘party’ can cause inflammation and infection in the tissues surrounding the dental implant. Various systemic diseases such as diabetes and certain lifestyle choices like smoking can also contribute to the development of peri-implantitis.
Risk Factors
Now that we know the causes, you might be wondering what puts you at risk? Several factors can increase the likelihood of developing peri-implantitis:
- Poor oral hygiene: Not maintaining your oral hygiene routine can lead to bacterial build-up, which, as we’ve seen, can lead to the infection.
- Smoking: Smoking not only affects your lungs but your oral health too. It can increase the risk of peri-implantitis.
- Previous history of periodontal disease: If you’ve had gum disease in the past, you’re more likely to develop peri-implantitis.
- Uncontrolled diabetes: Diabetes that’s not well-managed can pose a higher risk of peri-implantitis.
Despite these risk factors, remember that regular visits to your dentist, a well-maintained oral hygiene routine, and controlling other systemic health issues can help reduce the risk of peri-implantitis significantly. There’s no need to be afraid of going for that dental implant procedure you’ve been considering. 🤗
After all, knowledge is power! Understanding what peri-implantitis is, its prevalence, causes, and risk factors can empower us to take the necessary measures and keep our dental implants, and the smiles they support – healthy and sparkling. ✨🦷✨
Gum Disease and Bone Loss Impact on Dental Implants
Taking care of your oral health is much more than just keeping your smile bright and beautiful. It’s an integral part of maintaining your overall well-being. Among the various oral health issues, gum disease holds a notorious reputation. If left unchecked, it’s capable of leading to significant bone loss in the jaw, influencing the stability of dental implants. In this section, we delve into exploring how gum disease and bone loss affect dental implants.
Consistent oral hygiene basics from a young age, such as proper brushing and flossing techniques, are critical to preventing the onset of gum disease. However, despite our best efforts, many people may face this condition at some point in their lives.
Gum disease begins benignly as gingivitis but can progress to a more severe periodontitis if not addressed timely. In the latter stages, the gum begins to pull away from the teeth, creating pockets that are prime real estate for bacteria. These harmful pathogens can then make their way to the bone, causing inflammation and, eventually, bone loss.
When dental implants are on the table, the jaw bone’s health becomes crucial. Here, quality trumps quantity. It’s not just about having enough bone but about having healthy bone for proper implant integration and stability. Herein lies the conundrum:
- When the jaw bone suffers due to gum disease, it may not provide the necessary support for dental implants.
- Unhealthy bone may not fuse correctly with the implant, leading to failed integration.
- Ailing gums can also compromise the success of the implant, making post-operative healing a challenge.
“A stitch in time saves nine” – nowhere does this adage hold more truth than oral health maintenance. In our battles against gum disease and consequent bone loss, prevention truly is the best cure.
Regular dental check-ups, along with disciplined oral hygiene, can go a long way in warding off the nasty impacts of gum disease. When we nip this issue in the bud, we secure not only a radiant smile but also a healthier future, opening up possibilities for stable dental implants, if needed.
In the sprawling landscape of oral health, knowledge is power. Understanding the profound impact of gum disease and bone loss on dental implants equips us to take more proactive steps in our dental care journey. So, let’s keep the conversation going and bring about a revolution of responsible, informed, and proactive care for our pearly whites! 🦷💪
Links Between Gum Disease and Other Health Risks
We often overlook our oral health, focusing more on the aesthetics of a bright smile 🦷. Yet, there’s alarming research that indicates not prioritizing our oral health can have more severe repercussions than we thought. Shall we dive deeper and explore the connection between gum disease and an increased risk of heart disease, diabetes, and stroke?
Heart Disease
Gum disease and heart disease might seem unrelated at first glance. Nevertheless, studies reveal that individuals with gum disease are up to twice as likely to develop heart disease conditions. The culprit? Bacteria present in gum disease that find their way into our bloodstream. From there, these microbes latch onto fatty plaques in the heart blood vessels, leading to atherosclerosis (blocked arteries), an important factor behind heart disease.
Diabetes
If heart disease didn’t surprise you, this next link might. Gum disease is not only a potential result of diabetes but it can actually contribute to its onset. The oral infections that gum disease causes can elevate blood sugar levels, leading to increased periods of time when the body functions with a high blood sugar. This then increases the risk of diabetic complications. This cyclical relationship between gum disease and diabetes underscores the significance of good oral hygiene, including consistent Preventative Dentistry Practices.
Stroke
Last but definitely not least, let’s talk about strokes. Infections and inflammation from gum disease can cause the hardening of arteries, known as atherosclerosis, leading to blockages and blood flow problems that increase stroke risk.
Unfortunately, the links between heart disease, diabetes, stroke, and gum disease are all too real. Paying attention to your oral health is not simply about maintaining a pearly white smile, it’s about protecting, literally, your entire body health. A simple visit to the dentist has far-reaching implications beyond just warding off a toothache—it can potentially save your life. So remember, prevention is key! Regular brushing, flossing, and dental check-ups are non-negotiables for overall well-being. Don’t procrastinate; take that first step towards better oral hygiene now!
Dealing with Gum Disease When Considering Dental Implants
Never let gum disease stand between you and your dream of a million-dollar smile! 🚫🦷 Yes, it’s entirely possible to get dental implants even if you’re battling gum disease. However, like any good battle strategy, you need to get your troops (in this case, your gums) in the best shape possible to prevent any complications.
Gum disease, also known as periodontal disease, is a sneaky enemy. It creeps up, painless at first, gradually damaging your gums and the bones supporting your teeth. Untreated, gum disease could mean waving goodbye to your natural teeth. 😞 But don’t fret! A gum condition, however severe, does not disqualify you from getting dental implants.
Before you embark on your dental implant journey, though, it’s crucial to get gum disease under control. You don’t want to plan a major party (hello, new implants) without tidying up your house first, right? Think of treating gum disease as the essential cleaning that paves the way for those shiny new guests (implants) to settle comfortably in your mouth.
Steps to a Healthy Implant Journey
Here are the steps you need to follow to ensure your journey towards dental implants is as smooth as possible:
- Declare war on Gingivitis: This is the first step to maintaining a healthy mouth for implants. Aggressive brushing, flossing, and regular dentist visits for cleaning can reduce or remove plaque, the primary cause of gum disease.
- Seek professional help for periodontal disease: If your gum disease has escalated to periodontitis, talk to your dentist about treatments like root planing, scaling, or surgery.
- Monitor your mouth: Once gum disease is under control, it’s imperative to stay vigilant. Continue regular dental check-ups and maintain good hygiene habits at home.
- Prepare for implant surgery: After your dentist gives the all-clear, you’re ready for the implant procedure. Success rates for implants are high, but keeping gum disease at bay is key to longevity.
Remember, it’s not just about getting your smile back; it’s also about maintaining that smile long term. But with the right care, gum disease will soon be an enemy of the past, and that dream smile will be yours to keep. 🤩🦷✨
Conclusion
Knowledge is the key to prevention and the first step to treatment. Understanding how gum disease affects not only your oral health but also your potential to receive dental implants is crucial. Whether you’ve experienced gum disease or are implant-curious, knowing the risks and preventative measures can help make informed decisions about your oral health.
At Wilshire Smile Studio, we believe that everyone deserves a healthy, beautiful smile. Our dedicated team is here to help you understand your oral health and guide you through the best available treatment options, such as our highly successful dental implant procedures. With our affordable prices and personalized financing options, we make it easier for you to achieve your perfect smile. So, regardless of your past with gum disease, remember that our professional dentists are here for you. Don’t surrender to oral health problems when we’re just a call away. 😃
Remember, a healthy smile is more than just a mark of beauty—it’s a sign of great overall health. Let’s keep smiling together, healthy and bright!
Book your free consultation with us online or call (323) DENTIST (323-336-8478) today.
Frequently Asked Questions
1. What is gum disease?
Gum disease, also known as periodontal disease, is an infection of the tissues surrounding and supporting the teeth. It is often caused by poor oral hygiene and can lead to gum inflammation, gum recession, and tooth loss if left untreated.
2. How does gum disease affect dental implants?
Gum disease can negatively impact dental implants by causing gum recession and bone loss around the implant. This can weaken the implant’s foundation and ultimately lead to implant failure if not treated in a timely manner.
3. Can dental implants be placed if a patient has gum disease?
In most cases, it is recommended to treat gum disease before proceeding with dental implant placement. This ensures a healthy oral environment for successful implant integration. However, each patient’s situation is unique, and it is best to consult with a dental professional for personalized advice.
4. How can gum disease be prevented?
Gum disease can be prevented by practicing good oral hygiene, which includes brushing twice a day, flossing daily, using mouthwash, and visiting the dentist regularly for professional cleanings and check-ups. Avoiding tobacco use and maintaining a healthy lifestyle also contribute to gum disease prevention.
5. What treatments are available for gum disease?
The treatment for gum disease depends on its severity. It can range from professional dental cleanings and scaling to more advanced procedures like gum surgery and bone grafting. A dental professional will evaluate the condition and recommend the most suitable treatment plan.